Wondering how you should go about prenatal care in each trimester of your pregnancy? What healthy pregnancy habits should you build in each trimester, which will help you and your baby get the best results? Look no further because we have got you covered! In this blog, we’re going to look at how prenatal care differs in each trimester and some prenatal care tips you should adopt to have a healthy and fulfilling pregnancy.
Receiving quality prenatal and postnatal care is the most important factor in preventing complications during pregnancy and birth. Babies born to mothers who do not receive prenatal care are three times more likely to be underweight and five times more likely to die than those born to mothers who do receive care.
A pregnancy is divided into trimesters, as each trimester has a unique set of milestones and requires different prenatal care. The specifics of prenatal care differ depending on the trimester of pregnancy.
- the first trimester is from week 1 to the end of week 12
- the second trimester is from week 13 to the end of week 26
- the third trimester is from week 27 to the end of the pregnancy
First Trimester:
The first trimester starts before you become pregnant. It lasts from the first day of your last menstrual period until the 12th week of your pregnancy.
What you might feel:
Your first trimester of pregnancy brims with physical and emotional changes. This is an overwhelming time when you might have a lot of questions about the changes you’re noticing and about being pregnant. This is totally normal to feel this way. You may find yourself feeling moody, bloated and tired because of the hormonal changes happening in your body. During the first trimester, your uterus expands and your blood volume increases.
Here is what prenatal care you’d expect in your first trimester:
- Initial prenatal visit: During the first trimester, a woman will typically have her first prenatal visit, which includes a comprehensive physical exam and medical history, blood and urine tests, and an ultrasound to confirm the pregnancy and estimate the due date.
- Lifestyle counselling: You may be counselled about healthy eating, exercise, avoiding certain medications and substances, and any other lifestyle changes that may be necessary. You might be prescribed prenatal vitamins and supplements rich in Folic acid (a B vitamin) to ensure the proper development of your baby.
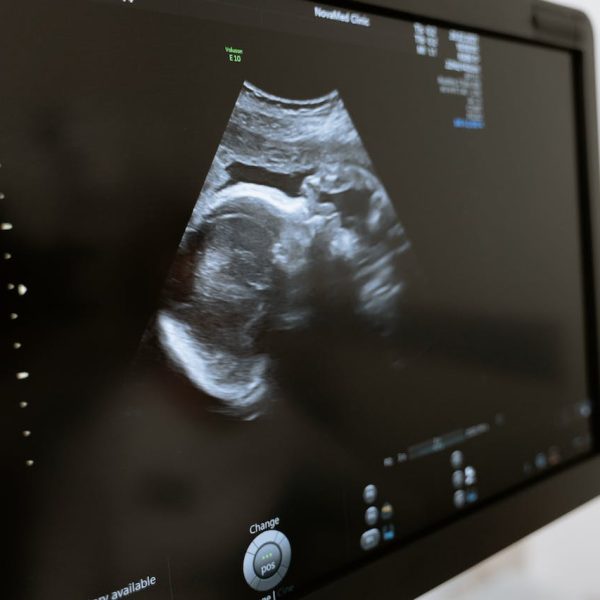
- Foetal development: The healthcare provider will monitor foetal growth and development through regular ultrasounds.
Read more: What are High-Risk Pregnancies?
Second Trimester:
In your second trimester, you will have a prenatal visit every month. The visits may be quick, but they are extremely important. Visits during this trimester will be a good time to talk about:

What you might feel and expect:
You might experience common symptoms during pregnancy, such as fatigue, heartburn, varicose veins, back pain and other aches and pains during the second trimester. You will start showing your pregnancy more. Your foetus has completed the development of all of its organs and systems and will now begin to grow in length and weight. Morning sickness usually subsides by this time, as do extreme tiredness and breast tenderness. You might start feeling more comfortable in your pregnancy as morning sickness usually subsides by this time, as do extreme tiredness and breast tenderness.
The following prenatal care might be followed in the second trimester:
- Tracking your baby’s development: During the second trimester, the healthcare provider will continue to monitor foetal growth and development through ultrasounds.
- Preparation for delivery: The healthcare provider may begin to discuss delivery options, including any special circumstances or preferences the woman may have.
- Assessing foetal movement: Notify your doctor when you start feeling flutters and kicks. Flutters are most likely to appear around 18 to 20 weeks of pregnancy.
During the second trimester, you might be offered various prenatal screenings or tests:
- Genetic tests: Blood tests may be offered to screen for chromosomal or genetic conditions such as spina bifida or Down syndrome. Your doctor might require you to undergo a diagnostic test, most likely an amniocentesis. A sample of the fluid that surrounds and protects a baby during pregnancy is removed from the uterus for testing during amniocentesis.
- Foetal ultrasound: Foetal ultrasound is an imaging technique that produces images of a baby in the uterus by using high-frequency sound waves. A detailed ultrasound can assist your doctor in evaluating foetal anatomy.
- Blood tests: Blood tests may be offered between weeks 24 and 28 of pregnancy to check your blood count and iron levels and screen for diabetes, which can develop during pregnancy (gestational diabetes). Blood tests also detect Rh incompatibility. Rh incompatibility occurs when a woman who is Rh-negative becomes pregnant with a baby with Rh-positive blood. The woman’s immune system reacts with Rh incompatibility and creates Rh antibodies. These antibodies drive an immune system attack against the baby, which the mother’s body views as a foreign object.
Third Trimester:
As you start the third trimester, your healthcare provider or midwife may change the schedule of your prenatal visits from every month to every 2 weeks. Your visits may be scheduled once every week in the last month and this will be based on your health condition, the growth and development of the foetus, and your provider’s preference.
What you might feel and expect:
The third trimester gets ready for the birth of your baby. The foetus’s weight and size continue to increase, and the body systems complete maturation. You may be feeling more uneasy now. You will continue to gain weight and will experience false labour contractions known as Braxton-Hicks contractions.
Here is what prenatal care you’d expect in your third trimester:
- Monitoring for complications: In the third trimester, the healthcare provider will monitor for any signs of complications, such as preeclampsia (high blood pressure), preterm labour, or foetal distress.
- Preparation for delivery: As delivery approaches, the healthcare provider will discuss the woman’s birth plan and any concerns she may have. Your provider might tell you to do some exercises to build your pelvic floor muscles to get you ready for labour and delivery.
- Foetal positioning: The healthcare provider may monitor the position of the foetus and discuss techniques to encourage optimal positioning for delivery. If your baby is rump-first or feet-first after week 36 of pregnancy, he or she is unlikely to turn headfirst for labour. An external cephalic version might be performed in this case, which is a procedure used to turn a baby from a breech position to a head-down position. Your doctor will apply pressure to your abdomen and physically manipulate your baby into a head-down position. If this procedure is not performed, or if your baby remains breech, your doctor might have to do a C-section delivery with you.
- Breastfeeding education: Breastfeeding is best for your baby. Talk with your healthcare provider about the benefits of breast milk. Education on breastfeeding and preparation for postpartum care may be provided to get you comfortable with breastfeeding your baby.
Read more: Myths of Pregnancy
Conclusion
Prenatal care is a critical aspect of a healthy pregnancy, and it should begin as soon as possible after a woman discovers she is pregnant. During the first trimester, prenatal care typically involves confirming the pregnancy, assessing the health of the mother and the developing foetus, and establishing a comprehensive medical history. During the second trimester, prenatal care focuses on monitoring the growth and development of the foetus, identifying any potential complications, and providing support and education for the mother. Finally, during the third trimester, prenatal care includes preparing for labour and delivery, monitoring foetal position and growth, and addressing any concerns that may arise. Overall, regular prenatal care can help ensure a healthy pregnancy, delivery, and postpartum recovery for both the mother and baby, and it is essential that pregnant women receive this care throughout all three trimesters.





















Share this article